What is an ERCP ?
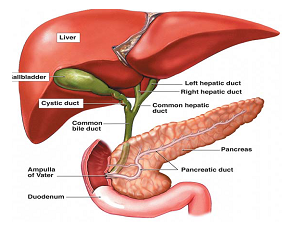 An ERCP is where the doctor examines the ducts of your liver, pancreas and gallbladder.
An ERCP is where the doctor examines the ducts of your liver, pancreas and gallbladder.
This is done by giving you some medication to help you relax. You will lie on the x-ray table on your tummy. The doctor will pass the endoscope, which is a thin, black flexible tube with a camera attached which allows the doctor to see the pictures as it is passed through your mouth, food pipe, stomach and into the first part of the small bowel.
A fine plastic tube will be passed down the endoscope and into the ducts of the liver and pancreas. A contrast material (dye) will be injected into the ducts and x-rays will be taken.
During the procedure, the doctor may remove stones and relieve the duct blockage.
This procedure may or may not require a sedation anaesthetic.

